Introduction
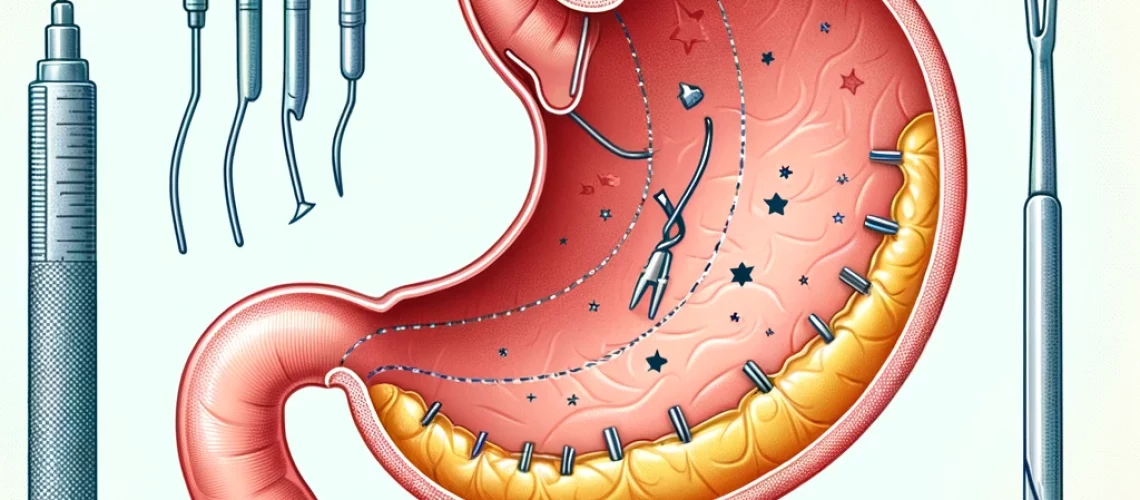
Gastric sleeve surgery, also known as sleeve gastrectomy, is a popular weight loss surgery that involves removing a large portion of the stomach to reduce its size and capacity. This restrictive procedure helps promote weight loss by limiting how much food can be consumed in one sitting.
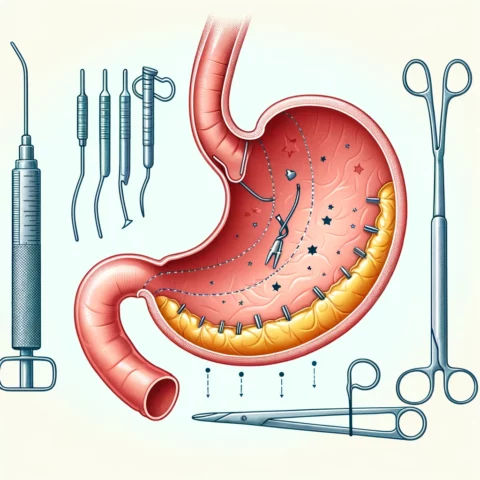
Gastric sleeve surgery has become one of the most common bariatric surgeries performed worldwide. According to the American Society for Metabolic and Bariatric Surgery (ASMBS), over 60% of weight loss surgeries in recent years have been sleeve gastrectomies. There are several reasons why this surgery has surged in popularity compared to other weight loss procedures.
Firstly, gastric sleeve surgery is less complex and invasive than other surgeries like gastric bypass yet still provides excellent weight loss results. The sleeve procedure only requires removing a portion of the stomach, whereas bypass also reroutes the intestines. This makes the surgery itself faster with a lower risk profile.
Secondly, the sleeve leads to favorable changes in gut hormones that suppress appetite, reduce cravings, and improve metabolism. Removing the portion of the stomach that produces the “hunger hormone” ghrelin plays a role in appetite reduction after surgery.
Lastly, the sleeve procedure only induces small amounts of malabsorption and nutrient deficiency unlike gastric bypass and duodenal switch surgery. This leads to more manageable long-term side effects and supplementation requirements.
The multitude of benefits make gastric sleeve an appealing option for those looking to lose a significant amount of weight and improve obesity-related health conditions. Sleeve surgery can help achieve sustainable long-term weight loss and put type 2 diabetes into remission while posing less surgical risk compared to more complex procedures.
Gastric Sleeve Surgery Procedure
Gastric sleeve surgery is performed laparoscopically, meaning it is minimally invasive. The surgery involves removing approximately 75% of the stomach along the greater curvature using surgical staples. This leaves a smaller, sleeve-shaped stomach about the size of a banana. The pyloric valve at the end of the stomach remains intact so that food passes normally into the small intestine after being eaten.
There are a few different techniques surgeons may use when performing sleeve gastrectomy:
- Standard laparoscopic sleeve: This involves using 5-6 small incisions in the abdomen to insert ports for the camera and surgical tools. The ports allow the surgeon to visualization the stomach and perform the sleeve resection laparoscopically.
- Single-incision sleeve: Also called SILS (single incision laparoscopic surgery), this uses only one incision through the belly button to insert the surgical port. The stomach is resected through this single entry point.
- Robotic sleeve: The surgeon performs the gastric sleeve using a robotic system that offers enhanced visualization and precision. Smaller surgical ports are used since the robotic arms are thinner than human wrists.
Regardless of technique, the end result is a smaller stomach pouch that limits how much can be eaten in one sitting to about 1-2 cups of food. This promotes early satiety and appetite reduction.
Risks and Benefits
Like any major surgery, gastric sleeve procedures carry some risks that need to be considered before undergoing the operation. Patients should discuss these risks thoroughly with their bariatric surgeon.
Some potential risks and complications of sleeve gastrectomy include:
- Leaks along the staple line of the remnant stomach
- Strictures or narrowing of the sleeve
- Blood clots
- Infection
- Vomiting and acid reflux after eating due to reduced stomach size
- Nutritional deficiencies if intake is inadequate after surgery
However, the benefits typically outweigh the risks for most patients. When successful, gastric sleeve surgery can provide impressive and sustainable weight loss results. Additional benefits may include:
- Loss of 50-75% of excess body weight within 1-2 years
- Significant improvement or remission of obesity-related diseases like type 2 diabetes and high blood pressure
- Reduced risk for heart disease, stroke, and certain cancers
- Improved mobility, energy levels, and quality of life
- Discontinuation of medications for diabetes, high blood pressure, high cholesterol, etc.
- Increased life expectancy
For this reason, bariatric surgery is considered the most effective intervention for significant long-term weight loss and reducing mortality in individuals with severe obesity or BMI over 40. Gastric sleeve, in particular, provides excellent outcomes with lower risk compared to more complex procedures.
Preparation and Recovery
Patients will need to undergo extensive medical, dietary, and lifestyle evaluations before being approved for bariatric surgery. This is to ensure they are healthy enough for the operation and committed to making the dietary and behavior changes required for success after surgery. Specific steps to prepare may include:
- Meeting with a bariatric surgeon and dietitian to discuss goals, risks, lifestyle changes, etc.
- Undergoing a psychiatric evaluation to screen for eating disorders, depression, or other mental health conditions
- Stopping smoking for at least 6 weeks prior to surgery
- Following a pre-op diet to shrink the liver before surgery
- Fasting after midnight the night before surgery
- Arranging transportation and take 2-3 weeks off work for recovery
The hospital stay is typically 1-3 days after surgery. Patients will be on a liquid diet for 1-2 weeks post-op as the stomach heals. Pureed, soft, and then regular foods are slowly introduced over a period of 4-6 weeks. Vitamin supplements are required after surgery to prevent nutritional deficiencies.
It may take 4-6 weeks to fully recover from surgery and feel comfortable returning to normal activities. Exercise can usually resume after about 6 weeks. Most patients can return to work within 2-3 weeks if the job does not require heavy physical demands.
Long-Term Outcomes
When performed correctly on appropriate candidates, gastric sleeve surgery can produce impressive long-term weight loss and health improvements extending out 10 years or more.
On average, sleeve patients lose about 60% of their excess body weight within the first 1-2 years after surgery. Many are able to maintain 50-70% of their weight loss long-term provided they follow the recommended dietary and lifestyle changes.
A study examining 7 years of follow-up data found an average of 57% excess weight loss was maintained by patients at the 7-year mark. Complete remission rates of obesity-related diseases were as follows:
- Type 2 diabetes: 83% remission rate
- Hypertension: 68% remission rate
- Dyslipidemia: 66% remission rate
The same study found major improvements in quality of life and physical function scores as well.
Beyond the 7 year timeframe, some limited data suggests at least 50% excess weight loss can be sustained out to 14 years post-op. More long-term research is still needed. However, current evidence indicates metabolic and weight loss improvements are durable for many sleeve patients provided they adhere to the recommended dietary, exercise, and lifestyle changes.
Conclusion
Gastric sleeve surgery is an increasingly popular weight loss procedure that provides impressive results for obesity and related conditions like diabetes when performed correctly. By restricting stomach capacity, the sleeve promotes early satiety and appetite reduction that can lead to significant weight loss and health improvements.
The surgery does carry risks that need thorough discussion with the surgical team. However, the benefits typically outweigh the risks for severely obese individuals struggling to lose weight through other means. Patients who adhere to the dietary, exercise, and lifestyle changes after surgery are able to maintain 50-70% of their excess weight loss long term.
If you are considering bariatric surgery for medically complicated obesity, be sure to speak with an experienced bariatric surgeon. They can help determine if you are a candidate for gastric sleeve or another weight loss procedure that may help improve your health and quality of life. Explore further resources on bariatric surgery and diabetes and bariatric surgery qualifications.mple markdown.